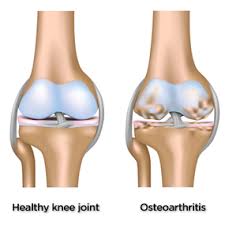
Injections of steroids into a joint to reduce pain and inflammation from arthritis is a relatively common practice. But this week, I read two studies that questioned this treatment…
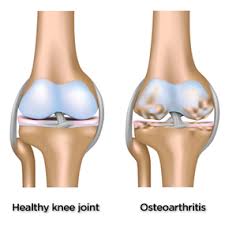
The first study compared knee injections of the steroid, triamcinolone, with saline and the injections were given every 12 weeks for 2 years. Although both groups experienced some pain relief, the difference wasn’t significant. And, the group that received triamcinolone had significantly greater cartilage volume loss than those who were injected with saline. Cartilage forms the natural cushioning layer inside our joints.
This study was published in the Journal of the American Medical Association on May 16, 2017.
The second study was reported in Univadis, a health news service I read every week, and the study was posted on Pubmed, a service of the National Health Institutes in USA. This study compared injections of sodium bicarbonate (baking soda) plus calcium gluconate, with injections of the steroid, methylprednisolone, given into the knee joint monthly for 3 months.
Although both groups showed benefit, the sodium bicarbonate/calcium group showed significantly greater improvement than the group who received the steroid injection. These results build on earlier research showing that bicarbonate/calcium injections were helpful for inflammatory joint disease, published in 2015 in BMC Musculoskeletal Disorders.
Taken together, these studies suggest that steroid injections should no longer be used to treat osteoarthritis, at least in the knee joint. Sodium bicarbonate and calcium gluconate are readily available in injectable form, are relatively inexpensive, and the second study suggests they may offer a beneficial substitute.
Sodium bicarbonate neutralizes acid, producing a more alkaline environment, and calcium acts as a buffer, also reducing acidity. So, in my mind, this begs the question: can osteoarthritis patients benefit from adjusting their diets to provide a more alkaline system? And would this help to reduce joint inflammation? Lots of health sites promote this as fact, but hard science is lacking, perhaps due to lack of funding to run proper studies.
However, the alkaline diet is a healthy one, consisting of whole fruits and vegetables, green juices and salads, beans and nuts. It is a plant-based diet that avoids added sugars, processed foods, excess meat and animal protein, and alcohol, caffeine and artificial sweeteners. Might be worth a try along with your doctor-recommended treatment – it seems highly unlikely a diet such is this could do any harm.
In fact, a diet similar to this is recommended for avoiding other chronic diseases like heart disease and diabetes so, whether or not you have arthritis, I’d recommend shifting your diet to contain more plant-based foods and less added sugar, processed food and animal protein. This brings me back to Michael Pollan’s recommendations I wrote about in an earlier blog:
-
Eat real food
-
Mostly plants, and
-
Not too much!
Simple rules to live by, and easy to follow!